Basal Thumb Arthritis: Types, Surgery, & More
What is Basal Thumb Arthritis?
Basal thumb arthritis is a type of osteoarthritis affecting the base of the thumb at the carpometacarpal joint. This joint consists of the articulation of a wrist bone called the trapezium with the first metacarpal bone, which forms the base of the thumb. The carpometacarpal joint is extremely mobile, allowing the pivoting and swiveling motions of the thumb, and essential for manipulation of the hand. This oft-used joint can become unstable and wear out over time. The ligaments can become lax and the cartilage of the joint can wear away causing pain and disability in susceptible individuals.
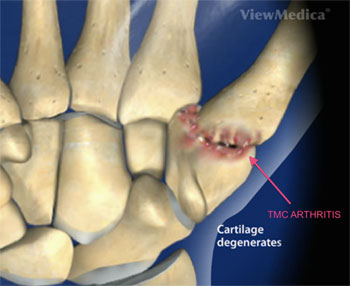
What causes Basal Thumb Arthritis?
The cause of Basal Thumb Arthritis is not known, however several risk factors have been associated with it. Like most forms of osteoarthritis, the incidence of Basal Thumb Arthritis increases with age, although it can also affect the very young. It is up to six times more common in women than in men, possibly due to ligamentous laxity associated with pregnancy and childbirth. Rheumatoid arthritis predisposes the basal thumb to arthritis. An occupation or hobby that involves repeated motion of the joint can cause degeneration of the joint. A history of trauma to the thumb, including Rolando’s or Bennett’s fractures of the base of the thumb have been associated with Basal Thumb Arthritis.
What are the symptoms of Basal Thumb Arthritis?
In the early stages of Basal Thumb Arthritis, pain may be present with activities such as writing, opening a jar, or twisting a doorknob. There may be tenderness and swelling over the carpometacarpal joint. As the condition progresses, the pain may increase in intensity and duration. A bony prominence may form at the carpometacarpal joint as a result of osteophyte formation, swelling and resulting misalignment of the joint. In late stages of the disease, weakness of grip, and inability to abduct or extend the thumb away from the hand are classic findings. Swan neck deformity of the thumb is a late finding.
How is Basal Thumb Arthritis Diagnosed?
Basal Thumb Arthritis is diagnosed with a careful history, thorough physical examination, and imaging studies. X rays with standard and stress views are employed to evaluate the joint. These views will assess joint misalignment (subluxation), joint space narrowing, osteophyte formation, and the condition of the cartilage. MRI may be used to help plan for surgery if indicated.
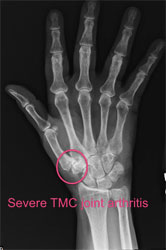
How is Basal Thumb Arthritis Treated?
Basal Thumb Arthritis can be treated non-surgically or surgically depending on the severity of symptoms and level of disability.
Non-Surgical
Resting the hand affected by Basal Thumb Arthritis is the first step in treating the condition. It is important to choose a specialized splint that immobilizes the thumb, such as a thumb spica splint. The splint is worn constantly, except for during bathing, for a period of a month. If improvement occurs, the splint may be removed at night and gradual weaning of the splint employed. NSAIDS may be prescribed during this time to treat any pain. A corticosteroid, can be injected into the carpometacarpal joint. This is highly effective, but cannot be repeated more than a few times as the steroid may have an adverse effect on the ligaments of the joint if not carefully used.
Surgical
Surgical treatment of Basal Thumb Arthritis is reserved for cases which fail conservative methods and cause substantial disability and pain to the patient. There are several surgical techniques to choose from. One method involves debriding the joint to create a new articular surface and then pinning it together, allowing fusion of the bones. While this accomplishes realignment and stops the pain, it also holds the metacarpal and carpal bone in a fixed position, preventing movement.
Dr. Knight prefers to remove the trapezium and tether the thumb metacarpal with the most innovative material around: the Mini Tight Rope. This thin, strong surgical suture will allow movement of the metacarpals without the immobility associated with rods, pins, or screws once the joint has healed.
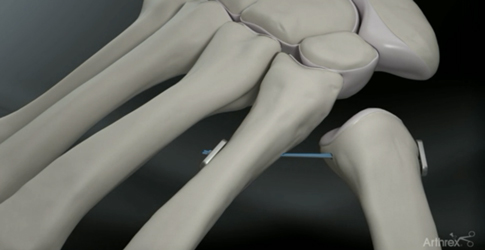
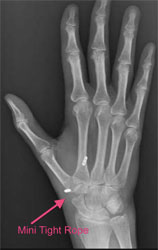
This procedure is done on an outpatient basis under general anesthesia. A cast is worn for 4-6 weeks after surgery and physical therapy is started once the cast is removed. Most patients will regain full range of motion using this advanced technique, a preferable outcome compared to basal thumb fusion procedures.
How can Dr. Knight help you with Basal Thumb Arthritis?
Basal thumb arthritis can be extremely painful, and Dr. Knight’s primary concern is to relieve you of this pain, as well as the accompanying inflammation, so that you can return to your life and work and continue to go about your daily routine with little or no change in behavior.
We looking forward to helping you live a more pain free life. Dr. Knight is one of the top hand doctors in Dallas. Contact us online, give us a call at (855) 558-4263 or visit Dr. John Knight at our Southlake hand and wrist center or Dallas office location.
Frequently Asked Questions:
How can I tell if I am developing thumb arthritis?
The symptoms of basal thumb arthritis are distinct, and as soon as you think you may have an issue in the joint, you should seek medical attention. The first thing you may notice is swelling and pain in the joint of the thumb, accompanied by aching and tenderness and loss of strength. There may also be a visible growth or bump at the joint as the result of bone spurs. A physical examination by the doctor will confirm this diagnosis.
Do I need surgery if I have thumb arthritis?
As with most hand conditions, surgery is always a possibility, but conservative treatment is the first line of defense to treat this condition. Osteoarthritis of the thumb is usually the result of a lack of synovial fluid in the joint which causes the two bones to rub together and this friction causes pain and inflammation. Usually, anti-inflammatory medication and splinting can help, but if it does not, then joint fusion may be necessary. This will lower your range of motion but get rid of the pain. In some cases, one of the small bones of the wrist, the trapezium, may be removed to stop pressure on the joint.
How can you test for thumb arthritis?
X-rays are a good first step in testing for basal thumb arthritis. These tests can ascertain the extent of the wear on the bones, as well as see if any bone spurs have developed because of the friction. A physical examination will also help the doctor determine the extent and the severity of your basal thumb arthritis.
Videos
Animated Videos
See how Dr. Knight incorporates the Mini Tight Rope in his repair, click on video below.
Surgical Video
Note: The following video contains graphic images.
(817) 382-6789
Disclaimer
HandAndWristInstitute.com does not offer medical advice. The information presented here is offered for informational purposes only. Read Disclaimer