Paronychia Treatment In Dallas
What is a Paronychia?
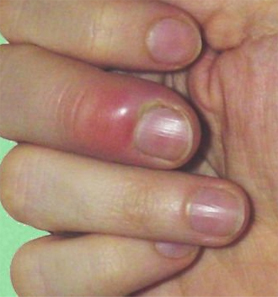
Paronychia is an infection of the folds of skin surrounding the fingernail. There are two types of paronychia: acute and chronic. While paronychial infections are typically mild in severity, they can be complicated by abscess formation, felon, or osteomyelitis of the finger. It is important to seek treatment for a paronychia early before complications develop. Diabetics and people who are immunocompromised are prone to more serious presentations of paronychia.
What causes a Paronychia?
Paronychia is caused by the invasion of a microorganism under the skin of the nail folds. Acute paronychia are typically bacterial in nature, while chronic paronychia are usually fungal infections, onychomycosis. Traumatic injury to the nail folds results in a break in the integrity of the skin, allowing entry of microorganisms. Some common sources of nail fold trauma include manicures, hangnails, and fingernail biting. Moisture can also compound paronychia by providing an ideal environment for bacteria and fungi to thrive. Children who suck their fingers may experience paronychia for this reason. Likewise occupations and hobbies which expose hands repeatedly to moisture may result in paronychia. Dishwashers, nurses, and swimmers are a few examples.
What are the symptoms of a Paronychia?
Acute paronychia presents with pain and swelling on a lateral nail fold. If an abscess is present, the area may be fluctuant, and a purulent discharge may be seen. Chronic paronychia presents with recurrent bouts of swelling of the nail folds. The proximal nail fold is typically involved. The symptoms are not as dramatic as seen with acute paronychia. Discomfort is present, and the affected area may have a spongy, boggy feel to it. Discharge is usually minimal, if present at all.
How is a Paronychia diagnosed?
Paronychia is a common infection and is usually diagnosed clinically based on a history of trauma to the nail fold and the symptoms described above. If drainage is present, it may be useful to perform a culture for bacteria and a KOH prep to identify any fungal elements to guide antimicrobial treatment. If herpetic whitlow is suspected, a viral culture would be useful to confirm the diagnosis. Imaging studies are generally not needed unless there is suspicion of a foreign body, fracture, or spread of infection to the bone.
How is a Paronychia treated?
Non-surgical
Minor paronychia, with redness, tenderness, and no fluctuant areas indicating abscess, can be treated with soaks. Epsom’s salts or Burrow’s solution soaks for approximately fifteen minutes three to four times a day may be all that is needed for the condition to heal. Soaks are useful in both acute and chronic paronychia.
If the paronychia involves more extensive redness without abscess, or if the patient is diabetic or immunocompromised, oral antibiotics oral antifungals will be needed in addition to the soaks.
Surgical
If an abscess is present, incision and drainage will be necessary. After the purulent material is removed, the wound will be irrigated and packed with gauze to allow healing to occur on its own. Sometimes removal of a portion of the fingernail may be needed.
How can Dr. Knight help you with Paronychia?
While not fatal (or even really painful), Paronychia can be an annoying ailment at best, and the fact of the matter is that no infection should go untreated, as it could possibly develop into other conditions that are far less benign. Should the infection spread into the bone, there could be very serious consequences, so it is best to treat quickly and fiercely to avoid this. Dr. Knight is well versed in treating these injuries, and will keep a simple infection from developing into something much more serious.
See Dr. Knight, one of the best hand surgeons in Dallas and see if he can help you live a more pain free life. Come to our Southlake hand and wrist center or Dallas Fort-Worth friendly office location.
Animated Videos
(817) 382-6789
Disclaimer
HandAndWristInstitute.com does not offer medical advice. The information presented here is offered for informational purposes only. Read Disclaimer